Introduction

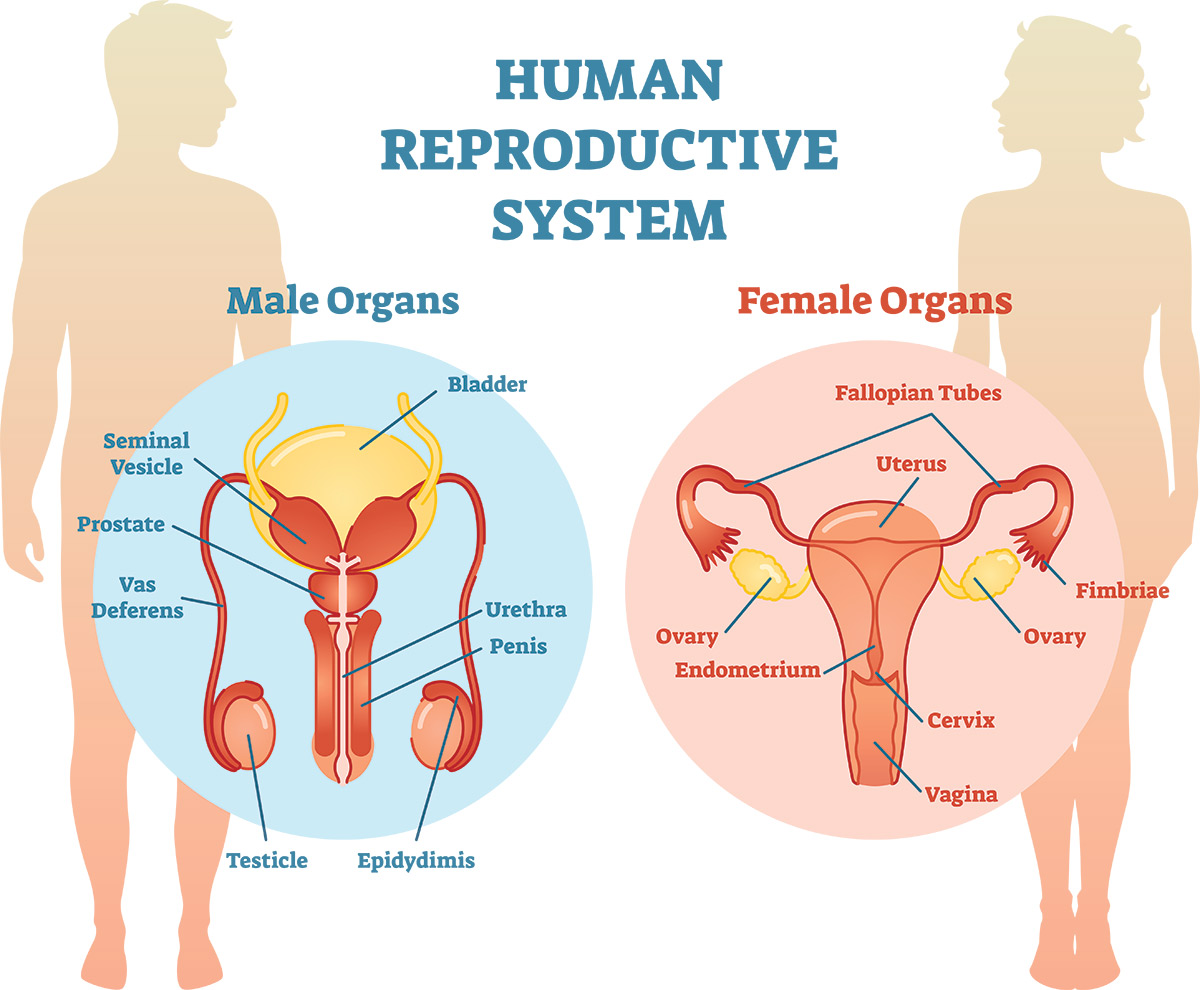
Reproductive health refers to the condition of male and female reproductive systems during all life stages. These systems are made of organs and hormone-producing glands, including the pituitary gland in the brain. Ovaries in females and testicles in males are reproductive organs, or gonads, that maintain health of their respective systems. They also function as glands because they produce and release hormones.
Reproductive disorders affect millions of Americans each year.
Female disorders include:
- Early or delayed puberty.
- Endometriosis, a condition where the tissue that normally lines the inside of the womb, known as the endometrium, grows outside of it.
- Inadequate breastmilk supply.
- Infertility or reduced fertility (difficulty getting pregnant).
- Menstrual problems including heavy or irregular bleeding.
- Polycystic ovary syndrome, ovaries produce more male hormones than normal.
- Problems during pregnancy.
- Uterine fibroids, noncancerous growths in a woman’s uterus or womb.
Male disorders include:
- Impotence or erectile dysfunction.
- Low sperm count.
Scientists believe environmental factors likely play a role in some reproductive disorders. Research shows exposure to environmental factors could affect reproductive health in the following ways:
- Exposure to lead is linked to reduced fertility in both men and women.1
- Mercury exposure has been linked to issues of the nervous system like memory, attention, and fine motor skills.2
- Exposure to diethylstilbestrol (DES), a drug once prescribed to women during pregnancy, can lead to increased risks in their daughters of cancer, infertility, and pregnancy complications.3
- Exposure to endocrine-disrupting compounds, chemicals that interfere with the body’s hormones, may contribute to problems with puberty, fertility, and pregnancy.4
-
Karen Clay, Margarita Portnykh, Edson Severnini. Toxic Truth: Lead and Fertility. 2019. NBER Working Paper No. 24607. [Accessed online 25 June 2019] [Available Karen Clay, Margarita Portnykh, Edson Severnini. Toxic Truth: Lead and Fertility. 2019. NBER Working Paper No. 24607. [Accessed online 25 June 2019]]
-
U.S. Environmental Protection Agency (EPA). 2019. Health Effects of Exposures to Mercury. [Accessed June 25, 2019] [Available U.S. Environmental Protection Agency (EPA). 2019. Health Effects of Exposures to Mercury. [Accessed June 25, 2019]]
-
American Cancer Society. 2019. DES Exposure: Questions and Answers. [Accessed June 25, 2019] [Available American Cancer Society. 2019. DES Exposure: Questions and Answers. [Accessed June 25, 2019]]
-
Endocrine Society. Impact of Endocrine-disrupting Chemicals on Reproductive Systems. [Accessed June 25, 2019] [Available Endocrine Society. Impact of Endocrine-disrupting Chemicals on Reproductive Systems. [Accessed June 25, 2019]]
What is NIEHS Doing?
NIEHS conducts and funds research to understand environmental factors that may affect human reproductive health.
Heat exposure during pregnancy – NIEHS-funded researchers studied more than 400,000 pregnancies and found that both long- and short-term maternal heat exposures during pregnancy are associated with increased risk of severe maternal morbidity. The Centers for Disease Control and Prevention lists 21 different indicators of this medical condition that unexpectedly occurs after labor and delivery. The prevalence of severe maternal morbidity has continued to increase in the U.S. despite improvements in improvements in prenatal care coverage and quality.
Heavy lifting or shift work and decreased fertility – Two occupational factors for women – lifting heavy loads or working non-daytime schedules – are associated with fewer eggs in their ovaries, which could indicate decreased fertility.5
Chemical exposure and assisted reproductive technology – Exposure to high levels of flame retardants6 and plasticizers7 may have a negative impact on the outcomes of in vitro fertilization (IVF), a technology used to help people get pregnant. The researchers found that women with higher levels of these chemicals in their urine had lower levels of ovary cells necessary for reproduction, and fewer successful pregnancies and live births.
Soy formula and menstrual pain – Girls who were fed soy formula as infants are more likely to develop heavy menstrual bleeding8 , severe menstrual pain9 , endometriosis10 , and larger fibroids11 later in life.
Vitamin D and uterine fibroids – Women with adequate levels of vitamin D are less likely to develop uterine fibroids than those with inadequate levels.12
Uterine cancer – Women who used chemical hair-straightening products were at higher risk for uterine cancer compared to women who did not report using these products, according to research from The Sister Study that included more than 33,000 women. The researchers found that women who reported frequent use of hair-straightening products, defined as more than four times in the previous year, were more than twice as likely to go on to develop uterine cancer compared to those who did not use the products. Uterine cancer is relatively rare and accounts for about 3% of all new cancer cases. But it is the most common cancer of the female reproductive system.
Sperm quality – A comprehensive study, which included systematic review and meta-analysis, found sufficient evidence of an association between higher insecticide exposure—organophosphates and methyl carbamates—and lower sperm concentration in adult males. People can be exposed to insecticides through residential, occupational, and recreational sources.
NIEHS-supported researchers found prenatal exposure to air pollution (PM2.5) may shorten the distance between the anus and genitals, or the anogenital distance. Anogenital distance is a way to gauge reproductive health related to hormone levels, such as testosterone. Shorter anogenital lengths in newborn males are an indicator of lower testosterone activity in the womb, which may have implications for fertility and semen quality in adults.
-
MÃnguez-Alarcon L, Souter I, Williams PL, Ford JB, Hauser R, Chavarro JE, Gaskins AJ; Earth Study Team. 2017. Occupational Factors and Markers of Ovarian Reserve and Response Among Women at a Fertility Centre. Occup Environ Med 74(6):426-431. [Abstract MÃnguez-Alarcon L, Souter I, Williams PL, Ford JB, Hauser R, Chavarro JE, Gaskins AJ; Earth Study Team. 2017. Occupational Factors and Markers of Ovarian Reserve and Response Among Women at a Fertility Centre. Occup Environ Med 74(6):426-431.]
-
Carignan CC, MÃnguez-Alarcon L, Butt CM, Williams PL, Meeker JD, Stapleton HM, Toth TL, Ford JB, Hauser R, EARTH Study Team. 2017. Urinary Concentrations of Organophosphate Flame Retardant Metabolites and Pregnancy Outcomes among Women Undergoing in Vitro Fertilization. Environ Health Perspect 125(8):087018. [Abstract Carignan CC, MÃnguez-Alarcon L, Butt CM, Williams PL, Meeker JD, Stapleton HM, Toth TL, Ford JB, Hauser R, EARTH Study Team. 2017. Urinary Concentrations of Organophosphate Flame Retardant Metabolites and Pregnancy Outcomes among Women Undergoing in Vitro Fertilization. Environ Health Perspect 125(8):087018.]
-
Hauser R, Gaskins AJ, Souter I, Smith KW, Dodge LE, Ehrlich S, Meeker JD, Calafat AM, Williams PL; Earth Study Team. 2016. Urinary Phthalate Metabolite Concentrations and Reproductive Outcomes among Women Undergoing in Vitro Fertilization: Results from the EARTH Study. Environ Health Perspect 124(6):831â839. [Abstract Hauser R, Gaskins AJ, Souter I, Smith KW, Dodge LE, Ehrlich S, Meeker JD, Calafat AM, Williams PL; Earth Study Team. 2016. Urinary Phthalate Metabolite Concentrations and Reproductive Outcomes among Women Undergoing in Vitro Fertilization: Results from the EARTH Study. Environ Health Perspect 124(6):831â839.]
-
Upson K, Harmon QE, Laughlin-Tommaso SK, Umbach DM, Baird DD. 2016. Soy-based Infant Formula Feeding and Heavy Menstrual Bleeding Among Young African American Women. Epidemiology 27(5):716-25. [Abstract Upson K, Harmon QE, Laughlin-Tommaso SK, Umbach DM, Baird DD. 2016. Soy-based Infant Formula Feeding and Heavy Menstrual Bleeding Among Young African American Women. Epidemiology 27(5):716-25.]
-
Upson K, Adgent MA, Wegienka G, Baird DD. 2019. Soy-based Infant Formula Feeding and Menstrual Pain in a Cohort of Women Aged 23-35 Years. Hum Reprod 34(1):148-154. [Abstract Upson K, Adgent MA, Wegienka G, Baird DD. 2019. Soy-based Infant Formula Feeding and Menstrual Pain in a Cohort of Women Aged 23-35 Years. Hum Reprod 34(1):148-154.]
-
Upson K, Sathyanarayana S, Scholes D, Holt V. 2015. Early-life Factors and Endometriosis Risk. Fertil Steril 104(4):964-9761. [Abstract Upson K, Sathyanarayana S, Scholes D, Holt V. 2015. Early-life Factors and Endometriosis Risk. Fertil Steril 104(4):964-9761.]
-
Upson K, Harmon QE, Baird DD. 2016. Soy-Based Infant Formula Feeding and Ultrasound-Detected Uterine Fibroids Among Young African-American Women With No Prior Clinical Diagnosis of Fibroids. Environ Health Perspect. 124(6):769-75. [Abstract Upson K, Harmon QE, Baird DD. 2016. Soy-Based Infant Formula Feeding and Ultrasound-Detected Uterine Fibroids Among Young African-American Women With No Prior Clinical Diagnosis of Fibroids. Environ Health Perspect. 124(6):769-75.]
-
Baird DD, Hill MC, Schectman JM, Hollis BW. 2013. Vitamin D and the Risk of Uterine Fibroids. Epidemiology. 24(3):447-453. [Abstract Baird DD, Hill MC, Schectman JM, Hollis BW. 2013. Vitamin D and the Risk of Uterine Fibroids. Epidemiology. 24(3):447-453.]
NIEHS Research Efforts
- Calorie Restriction, Environment, and Fitness: Reproductive Effects Evaluation (CaREFREE) – A study, conducted at NIEHS, that investigates how nutrition, fitness, and environmental factors affect women’s menstrual cycles.
- Environment and Reproductive Health (EARTH) Study – Conducted by grantees in Massachusetts, analyzes the effects of environmental contaminants on male and female fertility and pregnancy outcomes.
- LifeCodes – A pregnancy cohort, led by Brigham and Women's Hospital in Boston, providing samples and data from more than 5,000 pregnancies for research projects such as investigating the association between environmental exposures and spontaneous preterm birth. It is one of the nation’s largest pregnancy cohorts and specimen banks.
- Pregnancy And Childhood Epigenetics (PACE) – A consortium of researchers at NIEHS, and around the world, that studies how environmental exposures in early life affect pregnancy outcomes and child health.
- Reproductive System Disorders – NIEHS supports research that is developing a fuller understanding of the relationship between exposures and risk of reproductive health problems. For example, grantees are studying the effects of arsenic exposure on birth outcomes; ties between dioxin exposure and endometriosis; and the role endocrine disruptors might play in sperm chromosomal abnormalities.
- Study of Environment, Lifestyle, and Fibroids (SELF) – A study conducted at NIEHS that uses ultrasound screening to identify risk factors for uterine fibroid development in African-American women.
Further Reading
Stories from the Environmental Factor (NIEHS Newsletter)
- New Clues About a Birth Defect in Males Uncovered by NIEHS Scientists (January 2025)
- Early-life Exposures, Assisted Reproductive Technologies Can Alter Gene Expression, Says Falk Lecturer (November 2023)
- Risk for Female Reproductive Cancer May Increase After Early-life Exposure to Endocrine-disrupting Substances (November 2023)
- Exposures Affect Men’s Biological Clocks, Too (June 2023)
- Scientific Excellence, Mentorship Go Hand in Hand for NIEHS Researcher (June 2023)
- Anne Marie Jukic wins NIH Bench-to-Bedside award (January 2021)
- Early embryos develop successfully through molecule called tankyrase (June 2020)
- Humphrey Yao elected to board of Society for the Study of Reproduction (May 2021)
- On the road again: NIEHS shines at the Endocrine Society’s annual conference (July 2022)
- Researchers Identify Cells Involved in Development of Genitalia(July 2021)
- Preterm Birth, Prolonged Labor Influenced by Progesterone Balance (April 2021)
- Replacement Chemicals May Put Pregnancies at Risk (February 2020)
- Pregnancy Hypertension Risk Increased by Traffic-related Air Pollution (January 2020)
Fact Sheets
Cosmetics and Your Health: NIEHS Research Findings
Reproductive Health and Your Environment
Press Releases
- Preterm Birth More Likely With Exposure to Phthalates (July 11, 2022)
Podcasts
- Menopause and the Environment (2024) - NIEHS grant recipient Jodi Flaws, Ph.D., provides a brief overview of menopause and discusses her research that examines how exposure to phthalates may affect women’s reproductive aging. She also describes gaps in what we know about menopause and how research can inform clinical care to help women manage and treat their symptoms during the transition to menopause.
Additional Resources
- Common Reproductive Health Concerns for Women – Information and educational materials for women and health care providers provided by the U.S. Centers for Disease Control and Prevention (CDC).
- Journal of Women's Health Maternal Morbidity and Mortality – In the U.S., women are more likely to die from complications related to pregnancy or childbirth than in peer nations, and many health inequities are present among those who die. This special issue offers a research road map to help end this public health crisis. It showcases the work of NIH including NIEHS, other federal agencies, and the scientific community.
Related Health Topics
This content is available to use on your website.
Please visit NIEHS Syndication to get started.



